Article by Patrick Brennan, CEO, DetectedX
Radiologists often say that their ability to detect cancer is dependent on the quality of the mammogram. Radiology practices may take this a step further in that cancer detection rates also depend on the accuracy of the radiologists reading the mammograms.
The Mammography Quality Standards Act (MQSA) requires physicians who interpret mammography to obtain at least 15 hours of category 1 Continuing Medical Education (CME) units in mammography every 36 months to maintain their qualifications.[i]
Easy access to quality CME has always been a challenge for mammographers and facilities. Even before the pandemic, facilities had begun to question the value of conferences and broad training programs. Now, with travel constraints and staffing shortages, multi-day CME junkets are nearly out of the question. In this article, we discuss how on-demand breast education delivers both quality improvement and workforce development benefits. This can enable:
- practical pre-employment quality checks;
- ongoing professional development for existing staff;
- objective skills-based evaluation for annual auditing / QA reviews.
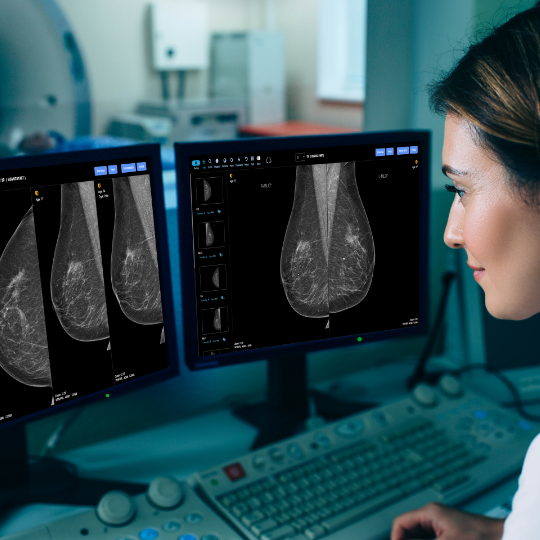
On-demand breast education delivers many benefits.
Better Accuracy for Better Care
High quality, accurate readings of mammograms are critical to the early detection of breast cancer. However, varying levels of skill and experience among radiologists can contribute to interpretation errors and variations, which can have a significant impact on patient care and outcomes. Easy access to high quality, on-demand breast education can deliver quality improvement, workforce development and improved outcomes for the clinician and facilities. The ultimate goal is to help radiologists diagnose breast cancer faster and more accurately, giving women worldwide a better chance of cancer survival.
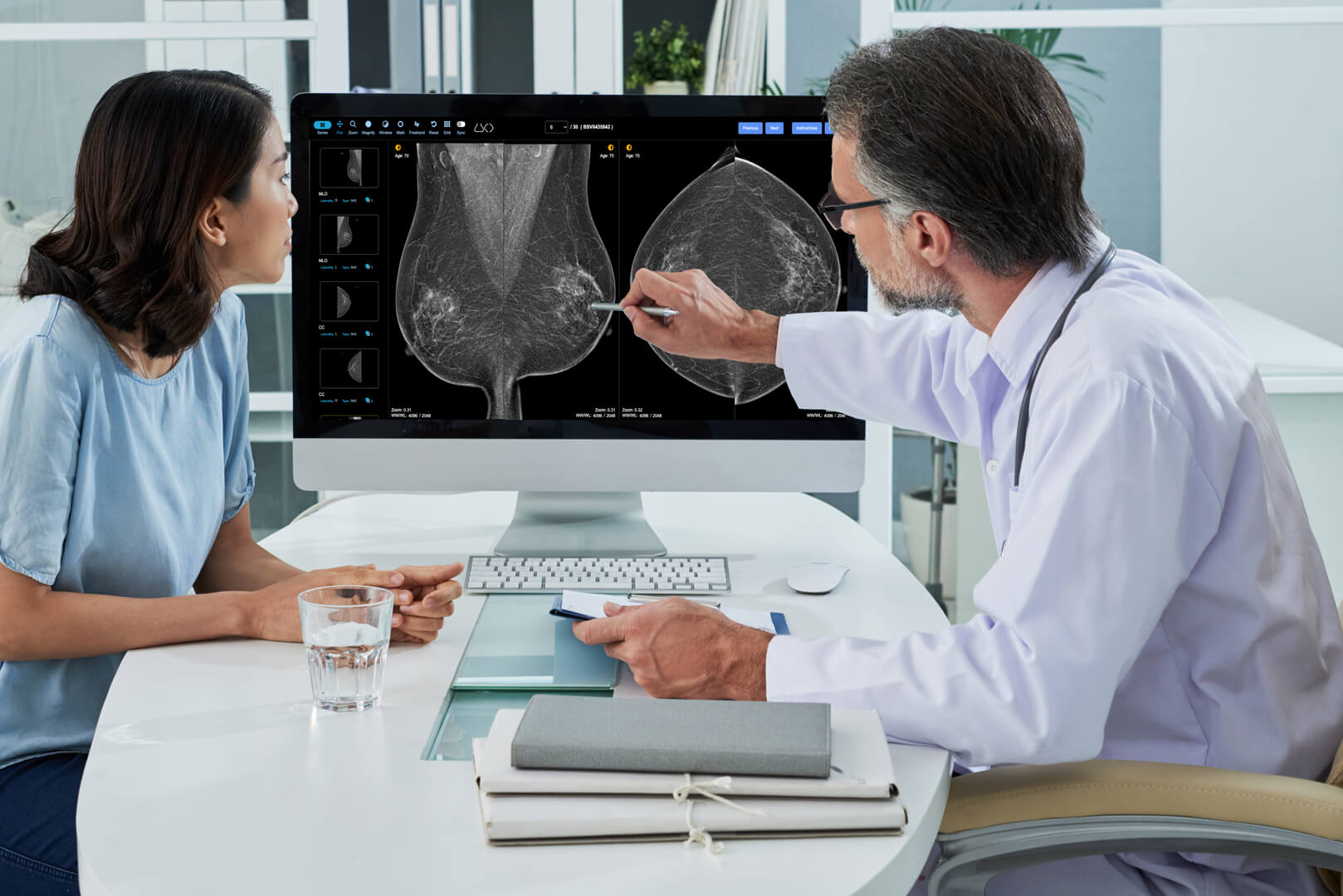
Education with Immediate Feedback is the Key
This is consistent with results associated with the DetectedX Radiology Online Learning Center, where use of on demand breast training has shown a 34% improvement in accuracy of diagnosing difficult cases. This on demand training is proven to help clinicians improve their ability to detect and diagnose breast cancer cases, significantly improving outcomes for patients.
By providing immediate feedback on discrepancies between truth and actual decisions, on demand training can be used to identify individual weaknesses and prescribe tailored education. This offers a cost- and time-effective way to meet CME requirements as well as accelerated learning, immediately improving outcomes for mammographers and facilities.
Practical Pre-Employment Quality Checks
False readings can create unnecessary trauma for patients and put practices at risk.[i] These risks can be reduced by making high quality training available for staff, as well as by comparing the performance of potential hires against existing staff or target accuracy rates. With instant feedback and certification, facilities have a tool to evaluate the diagnostic accuracy of potential candidates in an objective and practical manner.
Ongoing Professional Development for Existing Staff
DetectedX’s innovative educational technology enables radiologists to review, in real time, an enriched cohort of 2D mammography and Digital Breast Tomosynthesis (3D mammography) cases with varying levels of difficulty. The platform features real cases with full resolution images using real-life reading protocols and workflow. In their own reading environment, users view cases in DICOM format and can zoom and digitally adjust the images, including panning or adjusting window width and level.
The on-demand, online training packages provide immediate feedback on reading performance, comparing the user’s classification to the pathology-verified ground truth for each case. Using several metrics including sensitivity, specificity, true positive, true negative, false positive and false negative scores to gauge their performance, radiologists are able to identify errors and focus future trainings on areas of need to improve performance for earlier and more accurate disease diagnoses. Upon successful completion of each training module, users receive CME credits.
Objective Skills-Based Evaluation for Auditing and QA
Under MQSA, each mammography facility is required to perform a medical outcomes audit at least once every year. This is designed to track positive mammograms, correlate with pathology results and review known false-negative findings. Annual audits support continuous quality improvement at the facility and individual level – they also provide a tremendous opportunity for performance feedback.
Use of real cases that include both malignant and normal cases can be an effective supplement to clinical audits for assessing radiologists’ reading level and identifying areas for improvement. With confidential benchmarking, facilities have the ability to centrally store anonymized data to allow clinicians to compare their skills at local and national levels.
Variability in Radiologist Reporting and Methods to Improve Performance
Breast cancer screening shows wide variability among radiologists in the interpretation of screening mammograms.[i] While experience-related factors, such as annual reading volume, are frequently discussed as an explanation for variability among radiologists, few studies have shown a strong relationship. According to one study, breast cancer detection rates increased with the facility's screening-mammography volume but appeared to be unrelated to the radiologist's screening-mammography volume.[ii]
The persistent variability in reading performance has led to attempts to go beyond CME to generate improvement. An Institute of Medicine report suggested modifying the MQSA CME requirements to specifically focus on skills assessment using test sets with a mix of normal and abnormal findings. This assessment method would compare the performance of interpreting physicians with their peers to provide them with feedback on their interpretive skills and identify areas for improvement.[iii]
More recently, results from a randomized controlled trial suggest that interpretive performance can be improved by educational interventions based on actual clinical cases with findings that are frequently misinterpreted. These findings and the improvements in reading performance observed suggest that direct interventions focused on improving the accuracy of mammography interpretation should be the highest priority for meeting CME requirements under MQSA.[iv]
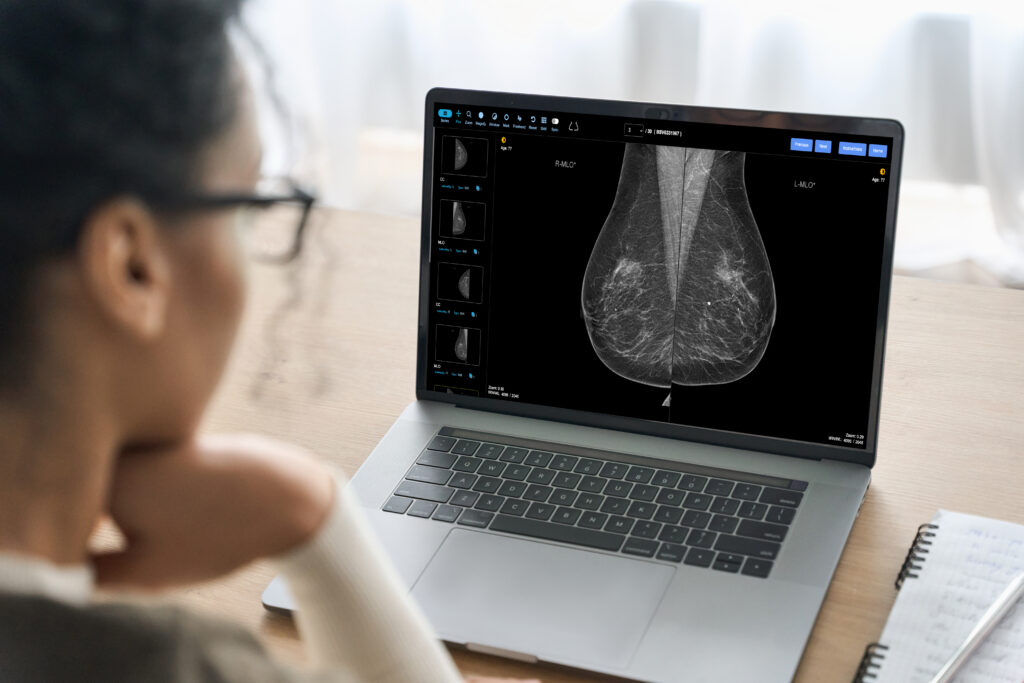
References
[i] Mammography quality standards act of 1992. Mammography facilities requirement for accrediting bodies, and quality standards and certifying requirements: interim rules (21 CFR 900) Vol. 58. Government Printing Office; Washington, DC: Dec 21, 1993. pp. 57558–72. Federal Register. 1992 1992. Report No.: 102-539.
[ii] Elmore JG, Wells CK, Lee CH, Howard DH, Feinstein AR: Variability in radiologists' interpretations of mammograms. N Engl J Med. 1994, 331: 1493-1499. 10.1056/NEJM199412013312206.
[iii] Isabelle Théberge, Nicole Hébert-Croteau, André Langlois, Diane Major, Jacques Brisson, Volume of screening mammography and performance in the Quebec population-based Breast Cancer Screening Program, CMAJ Jan 2005, 172 (2) 195-199; DOI: 10.1503/cmaj.1040485
[iv] Nass S, Ball J. Improving Breast Imaging Quality Standards. Institute of Medicine; Washington DC: 2005.
[v] Geller BM, Bogart A, Carney PA, Sickles EA, Smith R, Monsees B, Bassett LW, Buist DM, Kerlikowske K, Onega T, Yankaskas BC, Haneuse S, Hill D, Wallis MG, Miglioretti D. Educational interventions to improve screening mammography interpretation: a randomized controlled trial. AJR Am J Roentgenol. 2014 Jun;202(6):W586-96. doi: 10.2214/AJR.13.11147. PMID: 24848854; PMCID: PMC4276372.
[vi] Miller & Zois, citing Cannavale et al, 2013